Folic acid is the synthetic or man-made version of folate. It’s added to many fortified foods, multivitamins, and food supplements. Because of its widespread availability, individual consumption can often exceed the recommended limits. This leads to unmetabolized folic acid (or UMFA for short).
This blog post will answer the most common questions about UMFA. What it is, how it happens, what it does to the body, and what to do to prevent it from happening to you.
Table of Contents
What is unmetabolized folic acid (UMFA)?
As the name suggests, UMFA is folic acid (FA) that is NOT metabolized or converted to its bioactive form, 5-methyltetrahydrofolate or 5-MTHF (1).
Excessive folic acid intake (greater than 200 mcg) can add up – leading to a build-up of unmetabolized FA in the blood. Large doses exceed the capacity of the DHFR enzyme and overwhelm the liver’s metabolic capacity, too (2).
The following factors may affect folic acid metabolism and contribute to UMFA:
- Too much folic acid (more than the recommended amount – see table below for the list) from fortified foods and supplements
- Age and intestinal pH (can affect absorption rates, too)
- MTHFR genetic variation (affected individuals can’t do the conversion efficiently)
Is it necessary for folic acid to be metabolized?
Folic acid is a synthetic compound. As such, it has no biological function unless converted to its active form, 5-MTHF.
Once converted to 5-MTHF, this now-activated form can contribute to:
- the normal production of red blood cells
- homocysteine metabolism
- amino acid synthesis, and
- all the other benefits of folate
More importantly, women of childbearing age can increase their folate status. This is important to prepare and prevent neural tube defects (NTDs) in their developing fetus (3).
Related article: What is 5-MTHF? The Ultimate Guide to Folate and Methylfolate
Isn’t folic acid a water-soluble vitamin? If so, why is UMFA a concern?
Yes, folic acid is water-soluble and any excess you take is eventually excreted via urine. However, it’s important to note that folic acid metabolism does not occur instantly.
In small doses (less than 200 mcg), folic acid is rapidly metabolized and cleared from plasma via uptake into peripheral tissues. Some get flushed out via urine. But doses above the recommended 400 mcg daily can lead to detectable levels of UMFA in plasma.
In the 2007-2008 NHANES (National Health and Nutrition Examination Survey), UMFA was present in almost all serum samples! An astonishing 95% of the US population surveyed had UMFA concentrations greater than 0.3 nmol/L in their blood (4).
But that’s not all. In Ireland, a country without mandatory fortification, UMFA was found to be widespread amongst the elderly (5).

So, how did UMFA become so common?
It most likely began when folic acid fortification became mandatory. This vitamin was added to cereal, bread, pasta, rice, and other grains. The government launched this program with good intentions – to prevent NTDs in babies and save lives.
But here’s the kicker… people unintentionally started consuming too much folic acid. The excess folic acid intake led to unmetabolized folic acid. This isn’t surprising at all because the higher the folic acid intake, the more likely it is to have UMFA circulating in the body.
Here’s a brief timeline of FA fortification programs. Below, you can see when the UMFA started becoming a concern. It’s also apparent that the program works as expected when it comes to saving babies (6, 7, 8).
- 1992 – the US Public Health Service recommended that women of child-bearing age take 400 mcg of folic acid daily
- 1998 – the US and Canada introduced mandatory folic acid fortification. In the US, grain products manufacturers were required to enrich every 100g of flour with 140mcg of folic acid
- 2007 – in Canada, the FA fortification program helped reduce NTDs by up to 46%
- 2015 – a US study estimates that about 1,326 babies born without NTDs would otherwise have been affected without the program
- 2020 – more than 80 countries have implemented a folic acid fortification program
Related article: Why 5-MTHF Activated Folic Acid Is Best For Prenatal Health
Is unmetabolized folic acid a problem with naturally-occurring folate?
No, it isn’t. Folate and folic acid are absorbed differently by the body. Here’s a comparison of their absorption rates (1):
- Folate intake from food – about 50%
- Folic acid taken with food – about 85%
- Folic acid taken without food – nearly 100%
In short, folic acid is more readily absorbed by the body than folate.
The Food and Nutrition Board developed dietary folate equivalents or DFEs (9):
1 mcg DFE is equal to:
- 1 mcg food folate
- 0.6 mcg folic acid from fortified foods or supplements (when consumed with food)
- 0.5 mcg folic acid from supplements (when taken on an empty stomach)
What does this mean?
Since 1 mcg of food folate is equivalent to 0.6 mcg of FA, you need a lower dose of FA to get the recommended amount. So, for teens and adults, the recommended dosage is 400 mcg DFE. This means you will only need to consume 240mcg (with food) and 200 mcg (without food) of folic acid per day.

Is there a recommended folic acid dose to prevent UMFA?
Single doses of 100-200 mcg do not result in detectable UMFA levels in the blood, but 300-400 mcg does. Surprisingly, however, consuming smaller amounts of folic acid frequently can produce higher UMFA levels than taking the same total dose in larger, less frequent amounts.
Here’s the recommended daily amount for taking folic acid:
| Life Stage | Recommended amount |
| Birth to 6 months | 65 mcg DFE |
| Infants 7-12 months | 80 mcg DFE |
| Children 1-3 years | 150 mcg DFE |
| Children 4-8 years | 200 mcg DFE |
| Children 9-13 years | 300 mcg DFE |
| Teens 14-18 years | 400 mcg DFE |
| Adults 19+ years | 400 mcg DFE |
| Pregnant teens and women | 600 mcg DFE |
| Breastfeeding teens and women | 500 mcg DFE |
As for the tolerable upper limit (UL) of folic acid, it is set at 1,000 mcg/day.
The UL is defined as “the highest level of daily FA intake that isn’t likely to pose any negative health effects to almost everyone in the population”.
On the other hand, the lowest observed adverse effect level (LOAEL) is set to 5,000 mcg/day. The LOAEL is defined as “the lowest tested dose of FA that has been reported to cause adverse health effects”.
What are the adverse effects of unmetabolized folic acid?
Both excessive FA intake and UMFA may mask a vitamin B12 deficiency. It may also hide pernicious anemia. UMFA isn’t directly responsible for a B12 deficiency, but its capacity to mask the deficiency can delay treatment. If left untreated, this deficiency can damage the heart, brain, nerves, and cause digestive issues (10).
UMFA might also be linked to reduced numbers and activity of natural killer cells, which may harm immune health. These cells are the first line of defense against tumor cells and viral infections (11).
However, an in-vitro study contradicts the findings above. Researchers say that natural killer cell function is NOT influenced by either folic acid or 5-MTHF (12).
Another study says UMFA may cause cancer to accelerate or speed up (5). But there does not seem to be enough data to support this theory. For instance, a study that looked at 553 cases of breast cancer found that circulating UMFA is not associated with breast cancer risk (13).
So far, we’ve come across a bunch of seemingly conflicting studies…
Here’s an interesting theory that might explain why circulating UMFA (especially at low levels) may not be as harmful as originally thought:
As we all know, the human body is a complex machine that can adapt to many different situations. Well, one of them is UMFA circulating in the body. FA supplementation can indeed increase plasma concentrations of UMFA, BUT they do not remain elevated.
Moreover, there were no significant differences in the UMFA plasma concentration of women receiving 1.1mg vs 5mg of FA daily. This suggests that the body adapts to limit exposure to unmetabolized FA (2).
In summary, there may be potential adverse effects of UMFA. But further research is required before any definitive conclusions can be made.
Is there a way to prevent or avoid UMFA?
If you want to err on the side of caution and not risk excessive UMFA levels in your system, we suggest eating more foods naturally rich in folate, such as veggies, liver, bananas, eggs, and beans. Just be careful with food handling though. Folate is easily destroyed by incorrect storage, washing, and cooking.
Alternatively, consider taking the active form of folate/folic acid directly. The bioactive 5-MTHF form skips all the necessary conversions. This form is extremely helpful for people with the MTHFR genetic mutation. Taking 5-MTHF instead of folic acid also prevents any potential negative effects of circulating UMFA (14).
Check out this infographic highlighting the main differences between folate, folic acid, and 5-MTHF folic acid:
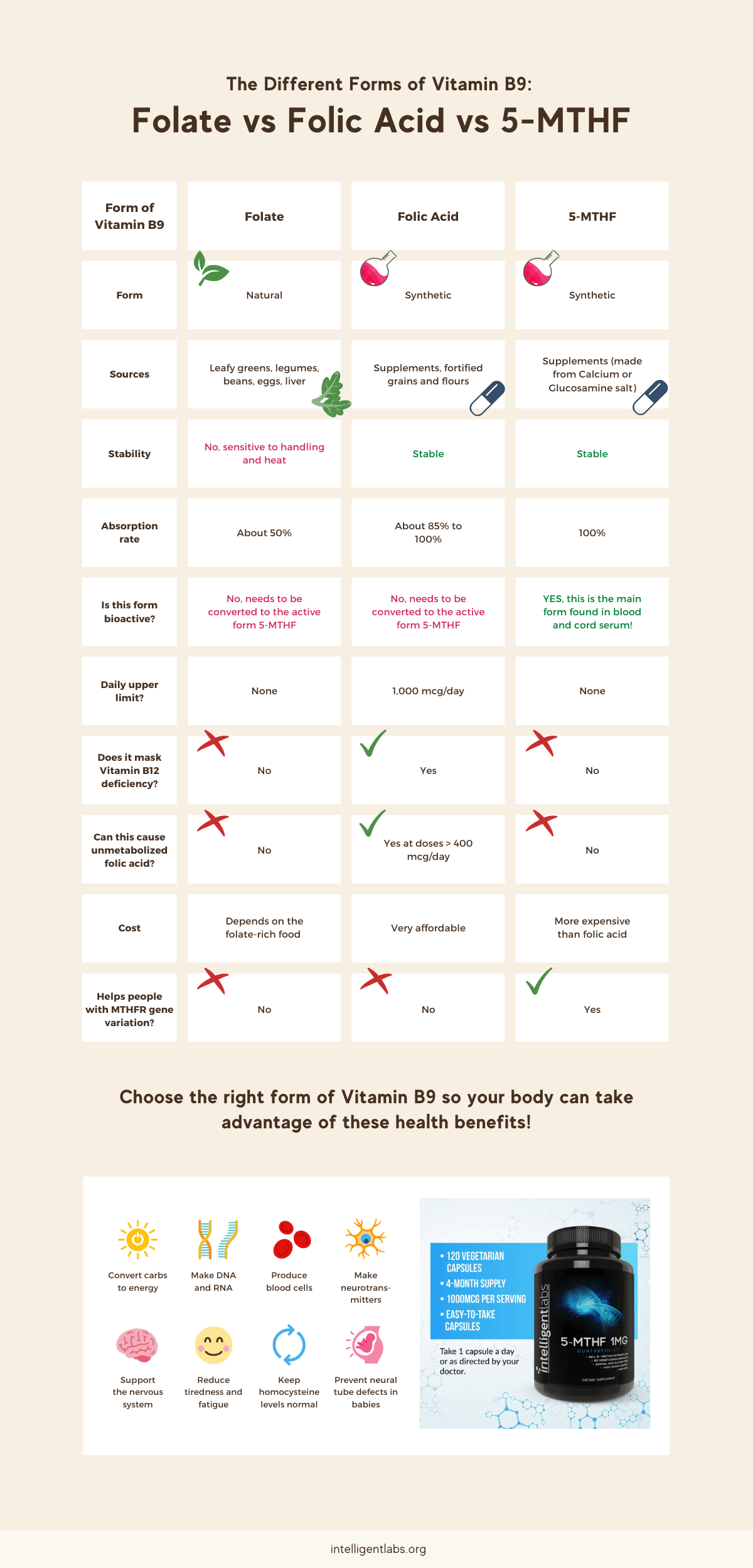
We recommend you check out our Intelligent Labs 5-MTHF activated folic acid supplements, made from non-shellfish Glucosamine salt for max absorption.
💬 Something on your mind? Share your thoughts in the comments. We love hearing from curious minds.
📩 And while you’re here, join our newsletter for more smart stuff (and secret perks)!
References
(1) The emerging role of unmetabolized folic acid in human diseases: myth or reality? Obeid R, Herrmann W. Curr Drug Metab. 2012;13(8):1184-1195.
(2) Circulating Unmetabolized Folic Acid: Relationship to Folate Status and Effect of Supplementation, Carolyn Tam, Deborah O’Connor and Gideon Koren, Published19 Feb 2012
(3) General Information About Neural Tube Defects, Folic Acid, and Folate, taken from: https://www.cdc.gov/ncbddd/folicacid/faqs/faqs-general-info.html
(4) Taken from JN The Journal Of Nutrition, https://jn.nutrition.org/
(5) Taken from The American Journal of Clinical Nutrition, https://ajcn.nutrition.org/
(6) General Information About Neural Tube Defects, Folic Acid, and Folate, taken from: https://www.cdc.gov/ncbddd/folicacid/faqs/faqs-general-info.html
(7) Folic acid food fortification in Canada. Ray JG. Nutr Rev. 2004;62(6 Pt 2):S35-S39.
(8) Updated Estimates of Neural Tube Defects Prevented by Mandatory Folic Acid Fortification — United States, 1995–2011, Jennifer Williams, MSN, Cara T. Mai, DrPH, Joe Mulinare et al.
(9) Folate, Fact Sheet for Health Professionals, from; https://ods.od.nih.gov/factsheets/Folate-HealthProfessional/#en70
(10) Taken from The American Journal of Clinical Nutrition, https://ajcn.nutrition.org/
(11) Taken from JN The Journal Of Nutrition, https://jn.nutrition.org/
(12) Natural killer cell cytotoxicity is not regulated by folic acid in vitro, Sandra Hirsch, Dante Miranda… Nutrition, Volume 29, Issue 5, May 2013, Pages 772-776
(13) Circulating unmetabolized folic acid and 5-methyltetrahydrofolate and risk of breast cancer: a nested case-control study. Koenig, K.L., Scarmo, S., Afanasyeva, Y. et al. Eur J Clin Nutr 74, 1306–1315 (2020).
(14) Folate, folic acid and 5-methyltetrahydrofolate are not the same thing, Francesco Scaglione, Giscardo Panzavolta, Pages 480-488 | Received 12 Jul 2013, Accepted 13 Sep 2013, Published online: 04 Feb 2014




